

More in Politics
-


Politics
Trump’s Attorneys Face Challenges: High Costs and His Unpredictable Actions Present Major Representation Hurdles
According to a recent report, the extensive legal team that former President Donald Trump has gathered...
-


Politics
Empowering the Fight Against Covert Drugging: Montana Law Amplifies Legal Stance on ‘Date-Rape Drugs
In a substantial legislative move, Montana enforces a new law designed to strengthen policies surrounding the...
-


Politics
Start of Trump’s $250 Million Civil Fraud Lawsuit: A Pivotal Moment in New York Court
The New York attorney general’s office has initiated a substantial $250 million civil fraud lawsuit against...
-


Politics
Trump Claims He Left a ‘Nice Note’ for Biden When He Left the White House in 2021
According to reports from The New York Post on Saturday, September 16, 2023, former President Donald...
-


Politics
Ivanka Trump Surprises Maui: An Unexpected Journey to Deliver Meals to Families
The Hawaiian island of Maui saw an unexpected yet wholeheartedly welcomed guest a few weeks back...
-


Politics
U.S. Calls for Public Assistance in Tracking Down Vanished F-35 Jet After Pilot Ejects
The U.S. military’s state-of-the-art F-35 jet has seemingly evaded its own team after a mishap led...
-


Politics
White House’s 9/11 Analogy for Biden’s Absence Raises Eyebrows
While President Biden marked the 22nd anniversary of the 9/11 attacks in Alaska, questions arose regarding...
-


Politics
Kamala Harris’s Bold Statement: ‘Ready to Assume Presidency’ if Biden Can’t Complete Term
U.S. Vice President Kamala Harris, on a diplomatic mission to Jakarta, responded to questions regarding President...
-


Politics
Controversy Shadows Medal of Honor Ceremony as Biden Exits Early
Tuesday’s Medal of Honor ceremony at the White House took an unexpected turn when President Biden...
-


Politics
Flames Erupt During Unauthorized Stunt Driving, Caught on Camera
A driver in Miami brought traffic to a standstill on an already congested holiday weekend by...
-


Politics
Trump Amplifies Anti-Trans Sentiment with Lady Weightlifter Impression
Donald Trump, aiming to resonate with conservative voters, once again showcased his anti-trans stance by performing...
-


Politics
Divergent Father’s Day Messages from Donald Trump and Joe Biden
President Joe Biden and potential 2024 Republican candidate Donald Trump both shared Father’s Day messages on...
-


Politics
Comer Admits Nobody Has Heard From Alleged Biden Informant for Three Years
James Comer, the Kentucky Representative chairing the House Oversight Committee, has conceded that the committee lost...
-


Politics
Trump’s Low Blow: Retaliating Against Chris Christie for Criticizing Ivanka Trump & Jared Kushner
Following Chris Christie’s announcement to challenge Donald Trump for the Republican Party nomination in 2024, the...
-


Politics
Trump’s legal team and Manhattan prosecutors are at odds about where he will stand trial
Ten months before Donald Trump’s historic New York City criminal trial, Manhattan prosecutors are using the...
-


Politics
Trump claims his supporters did not just gift him $5 million in 48 hours, more than 16,000 people joined as campaign volunteers within two days of his indictment
In the 48 hours following Trump’s indictment, his presidential campaign said it got $5 million in...
-


Politics
Trump raises his arrogance as legal barriers close in: ‘Like lighting a match’
Donald Trump is aware of the camera. He is particular about angles, lighting, and his signature...
-


Politics
The White House dodges the issue of whether the ‘assault weapons ban will result in ‘confiscation’
Karine Jean-Pierre, the White House press assistant, dodged a query Wednesday about whether President Biden’s planned...
-


Politics
Biden claims several Second Amendment claims in the aftermath of the Nashville shooting, but the reality is more complex
President Biden addressed Monday’s deadly school killings in Nashville, Tennessee during a visit to North Carolina...
-


Politics
Kimberly Guilfoyle Looks Beautiful in a Blue Dress After Defending Donald Trump
Kimberly Guilfoyle flaunted her figure in her most recent Instagram Story. On March 26, the conservative...
-


Politics
Trump threatens ‘possible death and devastation’ if he’s charged in hush money investigation
Former President Donald Trump increased his criticism against the Manhattan district attorney’s investigation into a hush...
-


Politics
Trump’s legal drama may push America closer to a historic turning point
Donald Trump’s legal situation seemed to worsen on Wednesday. The country moves closer to a political...
-


Politics
A judge orders Trump’s lawyer to testify in an investigation into classified documents: REPORTS
A federal judge quietly decided on Friday that Donald Trump‘s counsel must testify before a federal...
-


Politics
Federal authorities investigated Trump Media for alleged money laundering: Source
According to sources familiar with the matter, federal prosecutors in New York involved in the criminal...
-


Politics
Trump blames Mike Pence for January 6 riots on refusal to back a coup attempt
Donald Trump, whose coup attempt on Jan. 6, 2021, put his vice president’s life at risk...
-


Politics
Trump Adds Fuel to the Fire After Silicon Valley Bank’s Collapse
Former President Donald Trump fueled speculations of doom and gloom as he dove into the news...
-


Politics
After Bidens caused a stir by ordering the same dish twice while dining out, an etiquette expert weighs in
President Joe Biden and first lady Jill Biden both ordered the same rigatoni dish, sparking a...
-


Politics
Donald Trump’s Surprising Reaction to Losing Major Support: “I told Nikki to follow her heart”
South Carolina Republican Rep. Ralph Norman described Donald Trump as “benevolent” when he called to announce...
-


Politics
BBC announces the release of a new documentary and podcast on Kanye West
Kanye West’s “rollercoaster life and career” will be the focus of a new BBC documentary, which...
-


Politics
Trump Grand Jury Says Witnesses May Have Lied Under Oath: “All I want to do is this”
The special grand jury investigating former President Donald Trump’s efforts for re-election in Georgia in 2020...
-


Politics
Trump White House urged Twitter to remove Chrissy Teigen’s derogatory tweet against him
A former Twitter employee has given new insight into the company’s relations with the White House...
-


Politics
Trump seeking almost $1 million in fines for his ‘frivolous’ lawsuit against Hillary Clinton
Former President Donald Trump and one of his lawyers said Monday that they will appeal almost...
-


Politics
Biden administration intends to end COVID public health emergency in May
President Joe Biden of the United States has told Congress that on May 11, his administration...
-


Politics
Biden announced the United States would send 31 Abrams tanks to Ukraine
President Joe Biden stated on Wednesday that the US will send 31 Abrams tanks to Ukraine...
-


Politics
Trump hires a strong legal team to pursue former Manhattan prosecutor
Donald Trump has hired one of America’s best trial lawyers to go after a former Manhattan...
-


Politics
Former Trump Official to High School Students: “You have to do your part”
Roger Severino, the former director of the Office of Civil Rights at the Department of Health...
-


Politics
DC appeals court will decide whether E. Jean Carroll may sue Donald Trump for rape, being president makes him immune: Justice Department
The District of Columbia Court of Appeals heard arguments in former President Donald Trump’s appeal of...
-


Politics
Trump’s special counsel Jack Smith was given an “easy case” that could be “prosecuted at any time”
Former federal prosecutor Cynthia Alksne remarked on MSNBC’s “The Katie Phang Show” early Saturday morning that...
-


Politics
Kevin Mccarthy Must Commit To A Government Suspension Over Raising Of Debt Ceiling: Freedom Caucus Holdout
REP. KEVIN MCCARTHY would have to commit to “shutting down the government rather than raising the...
-


Politics
Suspect arrested in connection with New Year’s Eve machete assault on police officers near Times Square
The 19-year-old man suspected of using a machete to attack three police officers in Times Square...
-


Politics
‘Incredibly Damning Statements’: Former Prosecutor For Robert Mueller Sees Trouble For Trump
Former President Donald Trump rang in the new year at Mar-a-Lago with a New Year’s Eve...
-


Politics
Hughley asks for Donald Trump to be charged with manslaughter
Donald Trump, the former US president and current presidential candidate for 2024, did not conclude 2022...
-


Politics
Far-Right Republican Unloads on Marjorie Taylor Greene: You ‘Crossed a Rubicon!’
GOP infighting over who will become the next speaker appears to be boiling over. Far-right Rep....
-


Politics
Trump accuses “seriously troubled man” Kanye West of Invited White Supremacist to Dinner at Mar-a-Lago
Over the weekend, former President Donald Trump claimed that Ye, then known as Kanye West, invited...
-


Politics
Tucker Carlson presents Biden’s biggest blunders: ‘What did he just say?’
‘Tucker Carlson Originals: The Joe Biden Christmas Special’ is streaming now, exclusively on Fox Nation. This...
-


Politics
Bill Clinton Compared Donald Trump To Tony Goldwyn, Martin Sheen, And Michael Douglas
When asked a question on a late-night talk show, a former president took a dig at...
-


Politics
Barack Obama Reveals Favorite Movies, Music, and Books of 2022: “I always look forward to sharing my lists with all of you”
‘The Fabelmans,’ ‘The Woman King,’ ‘Tár,’ ‘Everything Everywhere All at Once,’ Lizzo, Bad Bunny, SZA, and...
-


Politics
Meghan McCain Responds to Being Called “Deranged” Over the “New York Times” Swastika Debate
Meghan McCain has reacted angrily to Eric Swalwell’s description of her as “deranged” in reaction to...
-


Politics
DeSantis’ recent education plan specifically targets teachers’ unions by eliminating automatic dues in favor of monthly mailed-in checks
Florida Republican Gov. Ron DeSantis announced Monday that he will sign bills increasing teacher salaries by...
-


Politics
Trump’s lawsuit over Mar-a-Lago search officially dismissed by a federal judge
A federal court in Florida dismissed former President Donald Trump’s complaint against the FBI for searching...
-


Politics
Republican representative sobbed as she begged her colleagues to vote against the bill allowing same-s*ex marriage
Rep. Vicky Hartzler of Missouri cried on the House floor on Thursday as she asked her...
-


Politics
Elon Musk’s feud with Donald Trump has continued after he criticized the ex-president’s call for the US constitution to be “terminated”
The billionaire just recently let the controversial mogul-turned-politician back on Twitter after his takeover after putting...
-


Politics
Trump asks for the Constitution to be abolished via Truth Social post
In a continuation of his election denial and promotion of fringe conspiracy theories, former President Donald...
-


Politics
Kimmel Makes Fun of Trump’s ‘Meeting of the Mindless’ with Kanye West & White Supremacist Nick Fuentes
Of course, you’ve heard about Donald Trump‘s recent dinner with Kanye West and West’s friend, white...
-


Politics
Republicans criticize Trump for meeting with ‘avowed racist’ Nick Fuentes, whom he blames on Kanye West
Republicans criticized former President Donald Trump for hosting controversial musician Ye (Kanye West) and white nationalist...
-


Politics
DeSantis Is Already Polling So Well for President That ‘He’s Only 5 Points Away From Trump Calling It Rigged’: Fallon
According to new polling, Florida Governor Ron DeSantis seems to be a credible challenger against twice...
-


Politics
Karine Jean-Pierre was criticized for shouting down reporters: “We have a process here. I’m not calling out on people who yell”
White House press secretary Karine Jean-Pierre faced further criticism from reporters and Twitter users alike after...
-


Politics
Trump Would Be ‘Well-Advised’ to Lawyer Up Before E. Jean Carroll Files Her Rape Lawsuit: Federal Judge
Attorneys representing writer E. Jean Carroll battled with the former president’s lawyer in federal court two...
-


Politics
USDA blames Russia for the increased price of Thanksgiving dinner
Russia’s ongoing war in Ukraine is one of the reasons your Thanksgiving feast will cost more...
-


Politics
Michael Cohen thinks Ivanka Trump’s self-exile from politics is due to her role as the FBI’s mole at Mar-a-Lago
Former President Donald Trump’s daughter Ivanka is withdrawing from politics because she and her husband, Jared...
-


Politics
Donald Trump responds as Elon Musk restores his Twitter account: “Truth Social is special!”
Donald Trump has been formally reinstated on Twitter, but the former president voiced concerns about his...
-


Politics
Trump announces his 3rd presidential candidacy: “We will be attacked”
Former President Donald Trump formally launched his candidacy for president in 2024, his third try. Trump...
-


Politics
Republicans question Biden’s homeland security chief in a possible preview of upcoming Congress: “Worldwide Threats to the Homeland”
Republicans chastised U.S. Homeland Security Secretary Alejandro Mayorkas at a congressional hearing on Tuesday and called...
-


Politics
Kari Lake blasts her Democratic opponent for not recusing herself as election chief despite her candidacy
Republican Arizona gubernatorial candidate Kari Lake blasted her Democratic opponent for failing to recuse herself as...
-


Politics
US awaits a decision on Biden in key polls As Trump prepares for a comeback bid: REPORTS
A polarized America braced for a tense night of election results and legal challenges on Tuesday,...
-


Politics
Ted Cruz hit with beer can during Astros World Series parade in Houston: man arrested
The senator from Texas was not hurt. The aggravated assault has been charged against a defendant....
-


Politics
Ken Griffin says it’s time to ‘move on from Trump, backs DeSantis for 2024
Republican mega-donor Ken Griffin believes it is time for the Republican Party to look beyond former...
-


Politics
Manchin demands Biden apologize for his ‘outrageous’ coal remarks
Senator Joe Manchin demanded Saturday that President Biden apologizes for saying coal plants “all across America”...
-


Politics
Hillary Clinton and other top Democrats filed a motion to sanction Trump for a ‘frivolous’ lawsuit
According to USA Today, former Secretary of State Hillary Clinton joined a number of other top...
-


Politics
Clinton demands Trump pay legal fees for blackmail lawsuit
Hillary Clinton wants former President Donald Trump to pay her legal fees after a judge dismissed...
-


Politics
Trump Should Be ‘Prosecuted’ After Pelosi Attack
Following the attack on Paul Pelosi, husband of House Speaker Nancy Pelosi, former federal prosecutor Glenn...
-


Politics
US Midterm elections 2022: Biden’s bad 2024 numbers improve, while Trump’s bad numbers get worse
A new USA TODAY/Suffolk University Poll finds that Americans are still not interested in a rematch...
-


Politics
Trump’s lawyers accept a court order from a House committee on January 6
The subpoena calls for the former president to testify either at the Capitol or by videoconference...
-


Politics
White House calls for weapon ban after St. Louis school shooting
“Every day that the Senate fails to send an assault weapons ban to the president’s desk...
-


Politics
Ted Cruz took shelter in a supply closet during January 6 riot: Book
Texas senator wrote he ‘vehemently disagreed’ with colleagues’ call to allow certification of 2020 election Ted...
-


Politics
WATCH: Trump Rally Crowd Suddenly Starts Singing National Anthem As He’s in Middle of Sentence About January 6
On Saturday, ex-President Donald Trump was speaking about the January 6 committee and Rep. Liz Cheney...
-


Politics
Legal Experts Evaluate Trump’s Latest Challenging Day in Court
A New York judge denied former President Donald Trump’s request to relocate the fraud lawsuit against...
-


Politics
Trump deposed in a defamation case filed by E. Jean Carroll: REPORTS
Former President Donald Trump testified under oath Wednesday in a lawsuit filed by E. Jean Carroll,...
-


Politics
Trump employee saw moving boxes on Mar-a-Lago security footage identified as former White House worker: REPORTS
A source confirms to CBS News that an employee at former President Donald Trump’s Mar-a-Lago resort...
-


Politics
WATCH: Marjorie Taylor Greene says she’s a victim of the Jan. 6 riot during the debate
Rep. Marjorie Taylor Greene (R-GA) accused her opponent for her seat in congress, Marcus Flowers, of...
-


Politics
Trump’s Truth Social violated the law, claims former vice president — who provided Feds with evidence: report
Federal investigators have received evidence of crimes from a former executive at the Trump Media &...
-


Politics
Trump threatened to reveal confidential sources in Russia investigation: Reports
Donald Trump considered revealing the identities of confidential official sources from his first impeachment, according to...
-


Politics
Legal Experts Applaud Justice Department’s ‘Compelling’ Response to Trump’s SCOTUS Appeal
A Department of Justice (DOJ) filing in response to former President Donald Trump’s request for the...
-


Politics
Mueller’s prosecutor claims Trump provided DOJ “damning evidence” at MAGA rally
Former President Donald Trump made it easier for the Justice Department to bring a criminal case...
-


Politics
Devastation after Russian bombs across Ukraine, as at least 11 dead in Kyiv: Video
The morning’s brutal attack on the Ukrainian capital of Kyiv was captured on camera from across...
-


Politics
Trump’s attempt to blame General Services Administration for Mar-a-Lago documents destroyed by new documents
An attempt by former president Donald Trump to blame the General Services Administration for having top-secret...
-


Politics
Trump caught in a lie after a new audio clip surfaced
In an interview with New York Times reporter Maggie Haberman last year for her upcoming book,...
-


Politics
Maggie Haberman claims lack of reporting ensures Trump escaped accountability
The 600-page book by New York Times reporter Maggie Haberman will be released on Tuesday at...
-


Politics
Trump disregards Hurricane Ian risks and refuses to reschedule a video-phone fraud deposition in Florida
Donald Trump refused to postpone a deposition in a class-action fraud lawsuit involving video phones, despite...
-


Politics
Marjorie Taylor Greene’s husband files for divorce: REPORTS
Perry Greene, the husband of far-right Rep. Marjorie Taylor Greene (R-GA), filed for divorce on Wednesday,...
-


Politics
Donald Trump Had Racist Reaction To Staff Members Of Color At White House: Book Claims
His chief of staff had to correct him. Donald Trump allegedly made a racist assumption about...
-


Politics
NY Music Festival: Nancy Pelosi booed during a surprise appearance
Mariah Carey, Metallica, The Jonas Brothers, and Usher performed at the festival On Saturday night, attendees...
-


Politics
Pro-Trump ‘Truth’ Rally Fizzles: Draws Almost As Many Opponents
According to multiple reports, only a few dozen people attended a right-wing January 6 “Truth” rally...
-


Politics
Trump’s aides were shocked by his ignorance and that he “knew nothing about so many things”
If his single term in office didn’t make it clear, Donald Trump wasn’t exactly prepared to...
-


Politics
How to Get a Refund for Student Loan If You Paid During Pandemic: Details
When President Joe Biden announced a plan to forgive student loan debt, many borrowers who had...
-


Politics
New footage shows fake Trump elector spent hours inside Georgia elections office the day it was violated: Reports
Newly obtained surveillance video showing a group of Trump supporters inside a restricted area of a...
-


Politics
Trump world bears down: ‘Every day feels like something else is piling on
The former president’s advisers fear that the DOJ probes are more expansive than publicly known. When...
-


Politics
Moscow Officials Urge Putin to GTFO: ‘Everything went wrong
As Moscow suffered yet another string of embarrassing losses in Ukraine this weekend, more and more...
-


Politics
Barack Obama and Wife Michelle Return to the White House
In attendance at the unveiling of their official portraits alongside President Joe Biden and First Lady...
-


Politics
Media Critics Not Buying Biden White House’s ‘Startling’ Efforts to Blame Trump for COVID School Woes
Trump’s push to reopen schools in 2020 was criticized by mainstream media outlets as being reckless....
-


Politics
Hillary Clinton claims that ‘suggestive’ upskirt photos inspired her to start wearing pantsuits
After “suggestive” photos of Hillary Clinton in a skirt were taken during her time as the...
-


Politics
Trump received hundreds of millions of dollars from his father’s real estate empire: ‘He lived off his parents’ money’
During a rally in Pennsylvania on Saturday, former President Donald Trump called Democrat candidate Lt. Gov....
-


Politics
Biden’s wandering speech takes a CREEPY turn when he notices a 9-year-old in the audience
On Tuesday, President Joe Biden set off more than a few perv-o-meter alarms when he abruptly...
-


Politics
Report: White House refuses to explain who will pay for Biden’s $500B student loan handout
Economists say taxpayers are likely on the hook for it. President Biden and White House officials...
-


Politics
Former White House adviser claims Biden administration is the “epicenter” of child trafficking
It is self-evident that open borders are harmful to the American people. Many illegal immigrants are...
-


Politics
Newly Released Trump Memo: ‘It Is Clear Why Barr Did Not Want the Public to See’
The head of CREW—which fought for the document’s release—said that “it twists the facts and the...
-


Politics
‘Benedict Donald’ Trump ‘Understood the Stakes in the Search Warrant That Was Executed’: MSNBC Panel
Donald Trump biographer Tim O’Brien explained that even though the former president “isn’t a sophisticated man”...
-


Politics
Trump Frantically Packed Up Documents to Take With Him After Finally Accepting He Was Leaving White House, Report Says
Between the January 6 Capitol attack, challenges to the 2020 election, and his impending second impeachment,...
-


Politics
FBI director makes First Public Comments after Raid on Trump’s Home
Christopher Wray, the director of the FBI, did not respond to investigations on Wednesday regarding an...
-


Politics
Trump Fields calls from Republican Allies to Speed up 2024 bid following FBI Raid
Top Republicans who have spent months trying to stop Donald Trump from starting another presidential campaign...
-


Politics
Lara Trump incorrectly says that Donald Trump had ‘every authority’ to take documents from the White House
Lara, the daughter-in-law of former president Donald Trump, spoke on Tucker Carlson. She discussed the FBI...
-


Politics
Trump says FBI agents raided his Mar-a-Lago Florida home: “not necessary or appropriate”
Classified material from Trump’s presidency was found at his Florida residence in February, a possible breach...
-


Politics
Photos in New Book Reveals First Look inside White House’s Private Rooms Redesigned by Melania Trump
The White House: An Historic Guide, a new book, is offering readers a view inside the...
-


Politics
Trump’s Impeachment Defense Lawyer has a Plan to Stop Him
Tuesday evening, as news broke that the deletion of the text message scandal had moved from...
-


Politics
Biden Tested Positive for COVID in ‘rebound’ case: “I’m still at work”
President Biden tested positive for COVID-19 in a “rebound” case on Saturday, according to the White...
-


Politics
Twitter Bursts over Kamala Harris’ use of pronouns “she/her” her self-introduction, Description of her Clothing
Tuesday’s dinner with Vice President Kamala Harris had her and others introducing themselves at the table...
-


Politics
Former Mike Pence Aides talk to federal grand jury as federal criminal probe of Trump picks up steam
Marc Short and Greg Jacob can provide firsthand accounts of Trump’s attempt to overturn the election...
-


Politics
Bill Clinton hails David Trimble as a leader of courage and vision
Former US President Bill Clinton has paid tribute to former Northern Ireland first minister Lord Trimble,...
-


Politics
Biden says Trump “lacked the courage to act” on January 6 riot: “You can’t be pro-insurrection and pro-cop”
President Biden claimed on Monday that on January 6, 2021, when Trump’s supporters overran the U.S....
-


Politics
Trump Says He Intended to Give Himself Congressional Medal of Honor but was told it was ‘Inappropriate’: ‘They Wouldn’t Let Me Do It’
After he flew to Iraq, the former president believed he was deserving of the honor awarded...
-


Politics
Donald Trump says if he decided not to run for political office the ‘persecution’ towards him would ‘immediately stop’
Former President Donald Trump claimed that Washington would leave him alone if he did not pursue...
-


Politics
White House: Biden Probably Carrying Highly Contagious COVID Subvariant BA.5
The BA.5 subvariant makes up to 80% of COVID-19 infections across much of the US. The...
-


Politics
Jill Biden Heckled by Unknown Bystanders at Connecticut Ice Cream Shop: ‘Your Husband is the Worst’
During a national summer learning tour, First Lady Jill Biden visited Connecticut, where hecklers shouted criticism...
-


Politics
Trump Had ‘Extreme Difficulty’ with His Speech the Day Following Jan. 6 Capitol Riot
According to sources familiar with the committee’s plans, the House committee looking into the uprising intends...
-


Politics
White House in Damage Control Mode as Joe Biden Says He ‘Has Cancer’: “had several localized, non-melanoma skin cancers removed with Mohs surgery”
Joe Biden regularly makes inaccurate remarks during his speeches which his critics believe proves his “mental...
-


Politics
‘The View’ Host Sunny Hostin Criticizes Biden for “Normalizing a Murderer” and fist-bumping the Saudi Crown Prince
Joe Biden’s choice to fist bump Saudi Crown Prince Mohammed bin Salman during a meeting on...
-


Politics
China threatens the United States with “forceful measures” if Nancy Pelosi visits Taiwan
(CNN) – China warned on Tuesday that, in the event that US House of Representatives Speaker...
-


Politics
Two persons were charged with a scheme to offer foreigners access to US leaders, including Trump
Two people have been accused of running a multi-year scheme that allegedly raised at least $27...
-


Politics
Donald Trump Arrives in New York City with Melania Ahead of Ivana’s Funeral Service
Two days prior to his first wife Ivana Trump’s funeral services, former President Donald Trump and...
-


Politics
Kinzinger says Jan. 6 hearing on Trump’s actions will “open people’s eyes in a big way”
Washington —Rep. Adam Kinzinger, a member of the House select committee looking into the assault on...
-


Politics
Kamala Harris loses 2 top assistants as VP’s office continues high turnover rate: “She has brought vision”
Domestic policy adviser Rohini Kosoglu and director of speechwriting Meghan Groob are leaving Vice President Kamala...
-


Politics
Mary Trump Says Donald Trump’s Mental Health is ‘Deteriorating’ Even More under Constant Attacks
Like the rest of us, Mary Trump finds it hard to comprehend that so many people...
-


Politics
AOC confronted a far-right troll on the Capitol steps who made vulgar remarks about her body: “I was actually walking over to deck”
Rep. Alexandria Ocasio-Cortez of New York criticized a far-right troll on Wednesday night who had earlier...
-
Politics
Trump criticizes Elon Musk, and says he could have made him ‘drop to his knees and beg’
Elon Musk has responded to former President Donald Trump’s allegation that he is too old to...
-


Politics
Obama Sent Fiery Email to Ex-White House Doctor After He Questioned Biden’s Cognitive Health
Obama told Jackson, who was the doctor for three presidents, that criticizing Biden’s mental state was...
-


Politics
Republicans are trying to ‘repeal the 20th century,’: Reagan’s lawyer
During a Wednesday appearance on MSNBC, Reagan White House Solicitor General Charles Fried explained how Republicans...
-


Politics
Meghan King Dating Businessman Trevor Colhoun after Separating From Cuffe Biden Owens
After her third unsuccessful marriage, Meghan King is now dating once more. Unnamed sources tell Page...
-


Politics
Trump’s 2024 campaign could change Midterm elections completely: Donald Trump doesn’t care about anybody else
Rumors are swirling that the ex-president could make an announcement soon, as January 6 revelations continue...
-


Politics
2 Officers Shot, Hundreds Flee During July 4th Fireworks in Philly: ‘Run, run, run’
“I didn’t hear the shots, but the cops were like, ‘Run, run, run,’” one woman told...
-


Politics
Trump warned ‘there’s more than one Cassidy Hutchinson’: Reports claim
Former White House aide Cassidy Hutchinson delivered devastating testimony about Trump’s actions and behavior on Jan....
-


Politics
Donald J. Trump, the meanest of the mean girls: “You don’t understand, Mike”
The testimony given on January 6 before the House committee has often been unreliable, mostly because...
-


Politics
The term ‘No-Look Handshake’ Trends on Twitter after Biden was Seen Shaking Hands with South Korea’s President without Making Eye Contact
At the NATO summit in Madrid on Wednesday, US President Joe Biden and his South Korean...
-


Politics
Kellyanne Conway says January 6 Committee Making Big Mistake not Cross-examining Witnesses
It’s pretty ‘remarkable’ Secret Service agents are willing to go under oath, says Conway Kellyanne Conway,...
-


Politics
Arizona’s Republican AG Tells Hecklers To ‘Shut The Hell Up
Trump has attacked Arizona attorney general Mark Brnovich for not doing more to support his efforts...
-


Politics
Country’s Richest People try to Influence the Illinois Race for Governor
In terms of political office, Illinois voters are seeing first-hand what money can buy. Tens of...
-


Politics
Biden signs gun control bill in wake of deadly mass shootings: ‘Lives will be saved’
Less than 24 hours after it passed through the Congress with unusual speed, President Biden signed...
-


Politics
Trump’s Vanity Could end up being a Major Gift to Jan. 6 Committee
We could soon find out if Trump and his family’s thirst for attention helped a filmmaker...
-


Politics
CBS News obtains images from documentary film footage given to Jan. 6 panel
The House select committee looking into the attack on the U.S. Capitol on January 6, 2021,...
-


Politics
Here is what Bill Clinton said in response to Donald Trump in “Late Late Show With James Corden”
When questioned on a late-night talk show, one former president made a jab at another former...
-


Politics
Joy Behar Had Few Words for Donald Trump’s White House Staff and Mike Pence on ‘The View’ Latest Episode: ‘Don’t Try and Fool Us’
On the most recent episode of The View, Joy Behar had a few words for Donald...
-


Politics
Trump’s Team Setting Up Eastman to Take Blame for Jan. 6
Trump in recent weeks has told confidants that he sees no reason to defend the lawyer...
-


Politics
Pence says he won’t let Dems use Jan. 6 ‘to distract’ from their ‘failed agenda’
Pence said he and Trump parted amicably, but that they have gone their separate ways. Former...
-


Politics
Texas GOP’s election denial underscores the ongoing threat that’s the central message of the Jan. 6 hearings
Last week, during a select committee hearing on January 6, the star witness warned that Donald...
-


Politics
Hillary Clinton Rules Out 2024 Bid: “I expect Biden to run”
‘I expect Biden to run… It would be very disruptive to challenge that…’ Hillary Clinton, a...
-


Politics
Barack Obama posts pic with Michelle, Malia, and Sasha on Father’s Day
Barack Obama celebrated Father’s Day by dropping an adorable picture featuring his wife, Michelle Obama, and...
-


Politics
President Biden Falls During Bike Ride: “I’m Good!”
Just as he rounded the corner to approach the pack, who wished him a happy Father’s...
-


Politics
Trump ‘Induced Murderous Rage’ In Insurrection Mob: It was “as dark as it gets”
They were ready to “tear Pence limb from limb.” It was “as dark as it gets,”...
-


Politics
Bill Clinton Gives Down-Home Advice On Persuading Other Side: “We gotta reach people where they live”
The former president offered tips on advocating for reasonable gun control on “The Late Late Show.”...
-


Politics
Hunter Biden’s ex-wife knew nothing of tax trouble: ‘I had buried my head in the sand’
Buhle claimed to have ‘buried [her] head in the sand’ about Hunter Biden’s financial ties to...
-


Politics
The January 6 committee calls Trump out for using false claims of election fraud to scam supporters
Committee says Trump campaign knew claims of election fraud were false but used them to raise...
-


Politics
Michelle Obama urges Voters to Stay Engaged in Anxious Times: “Our democracy is fading”
Michelle Obama urged Americans not to tune out of the nation’s stalemate political system on Monday,...
-


Politics
What to expect from the second Jan. 6 committee hearing: the committee will provide a “great deal”
On Monday, two panels of in-person witnesses will testify in front of a House committee probing...
-


Politics
Taking Aim at DeSantis, Trump Considers Launching 2024 Bid in Florida
In recent months, Donald Trump has told confidants that he may launch his presidential campaign for...
-


Politics
Trump Trapped By ‘Ego’ In 2020: “He can’t admit his tweeting and narcissism turned off millions”
The newspaper controlled by longtime Trump backer Rupert Murdoch called Jan. 6 “national shame” and ripped...
-


Politics
Ex-Obama Aide David Axelrod SKEWERS Joe Biden: “The presidency is a monstrously taxing job”
One of President Barack Obama‘s most trusted advisers has come out against President Joe Biden, the...
-


Politics
Arnold Schwarzenegger Revealed Donald Trump’s Hypocrite Behaviour Towards Him After One Phone Call: “Very Mean-Spirited”
Celebrity feuds are an exciting conflict to watch for people because of the recent social media...
-


Politics
‘Breaking’ Story About Biden Mtg In 2 Days Just Appeared On Trump’s Truth Social Account. True or False?
This was just posted on Twitter. I’m sharing it with the caveat that it’s likely that...
-


Politics
Report: Donald Trump to Testify In New York Probe Over Alleged Fraud In July
As per the lawsuit, NY State Attorney General Letitia James must complete her questioning by the...
-


Politics
No easy ride for Biden as Kimmel tells him to ‘start yelling at people
Serious questions on gun violence mean there are few laughs as US president meets late-night TV...
-


Politics
Biden’s ‘Childhood Stutter’ Excuse Comes Under Scrutiny
‘One of [Biden’s] aides gingerly asked whether I’d noticed the former vice president stutter during the...
-


Politics
Scandal-plagued Obama AG Makes Strange Prediction About America’s Future
Harold Hutchison on June 6, 2022. In a Monday interview, former Attorney General Eric Holder predicted...
-


Politics
Jill Biden was criticized for using foul slang in an interview
Jill Biden, M.D. While discussing her marriage with President, she inadvertently uttered a slang phrase with...
-


Politics
Former President Donald Trump To Terrorize Nation With 2024 Announcement Soon
Some advisers say it could come as early as this summer. If you lived from 2016...
-


Politics
Kyle Rittenhouse posts a video of himself firing off bullets from an automatic firearm: ‘Joe Biden, you’re not coming for our guns’
Kyle Rittenhouse tweeted a video on Monday showing himself firing what seemed to be an automatic rifle while telling President Joe Biden that he couldn’t take Americans’ guns away. Rittenhouse tweeted the video with the comment, “Come and take ’em, Joe.” The video appeared to show Rittenhouse unleashing a barrage of shots from an automatic rifle at a shooting range, as Yahoo reported. Rittenhouse offers a thumbs up after moving back from the pistol and being patted on the back and says, “Joe Biden, you’re not coming for our guns.” In August 2020, Rittenhouse fatally shot two individuals and injured a third during protests in Kenosha, Wisconsin. In November, he was cleared of five charges, including first-degree homicide. Biden urged government action on gun reform...
-


Politics
Trump is moving from Mar-a-Lago to New Jersey for the summer
Former President Donald Trump is leaving Florida to avoid the summer storms. According to a Republican...
-


Politics
Memphis City Council refuses to give Trump security: “He’s notorious for not paying”
Former President Donald Trump is scheduled to hold a campaign rally in Memphis, but the city...
-


Politics
Ex-Prosecutor Says Peter Navarro Bust Likely Warning To Trump Cronies DOJ Isn’t ‘Fooling around’
A former federal prosecutor said Saturday that the no-frills FBI arrest of Donald Trump‘s former trade...
-


Politics
Trump’s plans for summer include 7-hour grilling in his fraud case
Donald Trump and three of his children agreed to testify under oath for up to seven...
-


Politics
Biden Calls On Congress to Reinstate Federal Assault Weapons Ban and New ‘Red Flag’ Laws
On Thursday night, President Biden set out his gun-control agenda, stating that the policies he proposed...
-


Politics
Biden Blanks during Coast Guard Changing Of the Guard Ceremony, While CNN Captures Classic Fail Moment
On Tuesday, Joe Biden‘s brain was not functioning properly. During the Coast Guard changing of the...
-


Politics
Herschel Walker accuses Donald Trump of lying: “So, I’m mad at him”
“I’m mad at [Trump], because he never asked, but he’s taking credit that he asked.” Many...
-


Politics
Why Donald Trump Isn’t to Blame for America’s Toxic Political Tribalism
The man who wrote the definitive work on how Americans have become splintered by their politics...
-


Politics
Hunter Biden’s Shady Business Associates Frequently Visited White House, $5.2 Million for ‘the Big Guy’ Discovered
Hunter Biden’s business ties to his father Joe Biden’s administrations are becoming more clear, as his...
-


Politics
Ted Cruz Got Heckled At Houston Restaurant Following His Speech at NRA Convention in Which He Broadly Rejected Proposals for Gun Control Days after Uvalde School Shooting
Following the gun massacre in Uvalde, Texas, which claimed the lives of 19 children and two...
-


Politics
Kamala Harris calls for a ban on assault weapons: “An assault weapon is a weapon of war”
Vice-president demands action after speaking at funeral for Ruth Whitfield, oldest person killed in Buffalo shooting...
-


Politics
McCarthy escalates standoff with January 6 panel over subpoena: “I expressly reserve Leader McCarthy’s right to assert any other applicable”
Republican Leader Kevin McCarthy has made it clear that he will likely decline to appear in...
-


Politics
Donald Trump’s Media Company Plans to Build New Streaming Service ‘TMTG+’ As ‘Non-Woke Alternative’ To Netflix and Disney+
In a recent SEC filing, Donald Trump‘s media and technology firm stated that it will build...
-


Politics
Texas Gunman Left Home after Fight with Mom about Wi-Fi: “He was kind of a weird one”
The man who opened fire in a Texas elementary school Tuesday, killing 19 children and two...
-


Politics
Whoopi Goldberg criticizes audiences of ‘The View’ for booing Kellyanne Conway
Whoopi Goldberg, co-host of ABC’s “The View,” chastised studio audience members on Tuesday for taunting former...
-


Politics
‘The View’ Hosts Make Fun of Ted Cruz’s ‘Creepy’ Rage Over Pete Davidson’s Love Life
Ted Cruz’s concern about Pete Davidson’s love life amuses and disgusts the hosts of “The View.”...
-


Politics
Washington Post-Ipsos Poll Says 75 Percent of Black Americans Fear Being Physically Attacked Because of Race
According to a new poll, 75% of Black Americans are concerned that they or a loved...
-


Politics
Trump fined $110,000 for Obstructing Tax Inquiry
Former US President Donald Trump has paid a $110,000 (€104,000) fee for obstructing a significant tax...
-
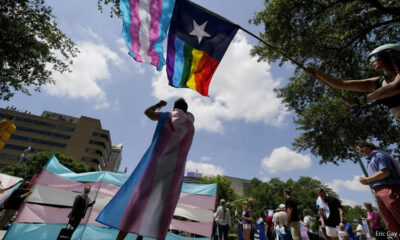

Politics
Texas Supreme Court Grants Partial win to Transgender Children
The Texas Supreme Court criticized the state’s governor and attorney general last week for circumventing conventional...
-


Politics
Melania Trump Talks about Her Critics and More in Her First Sit-Down Interview Since Leaving White House: “People I See Always Criticize Me”
Melania Trump gave her first sit-down interview since leaving the White House on Fox News on...
-


Celebrities
Former US First Lady Melania Trump Gives Explosive New Interview since leaving the White House
The former First Lady of the United States has given her first interview since leaving the...
-


Politics
Biden administration announces a $45 billion plan to connect the entire U.S to the internet by 2030
The Internet for All initiative is funded by the $1 trillion Bipartisan Infrastructure Law. The Biden...
-


Politics
Senate Democrats’ Bill to keep Abortion legal in the U.S Fails due to a GOP-led Filibuster
Sen. Joe Manchin joined all Republicans in voting to block the legislation, which Democrats want to...
-


Politics
Hunter Biden’s Tax Bill Supposedly Settled With $2 Million Loan from Hollywood Lawyer
Hunter Biden‘s tax issues were supposedly settled with a $2 million loan from a Hollywood lawyer...
-


Politics
Trump blamed Defense Secretary for Failing to Invoke Insurrection Act during BLM Riots: “You betrayed me”
‘Mark Esper was a stiff who was desperate not to lose his job… ‘ According to...
-
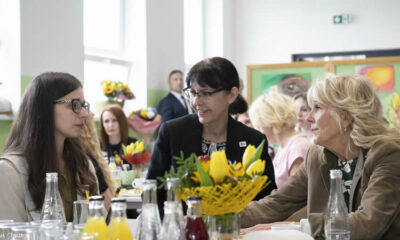

Politics
Jill Biden Pays Tribute to ‘Resilient’ Ukrainian Moms on Mothers’ Day: “Ukrainian Mothers, Like Svitlana, Continue to Be So Strong and Resilient”
“We stand with you,” Jill Biden said in a message to the families. She also thanked...
-


Politics
Kamala Harris Cautions That Women May Lose Right to “Make Decisions about Their Own Bodies” In Graduation Speech at Tennessee State University
Kamala Harris also cautioned graduates of Tennessee State about Russian aggression. In her graduation speech at...
-
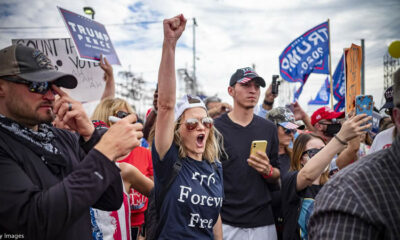

Politics
Study claims: Trump Supporters Use less Cognitively Complex Language and think in more Simplistic ways than Biden Supporters
According to new research published in the Journal of Social Psychological and Personality Science, Trump supporters...
-


Politics
Biden Slams GOP’s “Extreme” MAGA Agenda
In advance of the Midterm elections, the president, who ran on bipartisanship, takes off the gloves....
-


Politics
Bipartisan group urging House not to tie aid to Ukraine to COVID-19 funding: “Your fight is a fight for everyone”
A bipartisan group of U.S. military veterans in Congress has called on U.S. House Speaker Nancy...
-


Politics
Trump and his allies to campaign for Herbster at I-80 Speedway
A rally planned for Friday night in Greenwood in support of Charles Herbster’s bid to become...
-


Politics
Boeing CEO Dave Calhoun believes the company should have avoided Trump-era Air Force One deal: “Art of the Deal”
Boeing CEO Dave Calhoun told investors on Wednesday that the company should not have agreed to...
-


Politics
Florida can’t Dissolve the Special Tax District until the debt is Fully Paid: Disney Claims
The Reedy Creek special district made a statement last week indicating it would conduct business as...
-


Politics
Greene’s Text Messages Refocused Attention on his Martial Law Testimony
In a January 2021 text, Greene told Trump’s chief of staff that some lawmakers wanted the...
-


Politics
Federal Judge Temporarily Stopped Administration of President Joe Biden from Lifting Title 42 Covid Border Restrictions for Migrants
A federal judge in Louisiana has temporarily blocked the Biden administration from lifting a Trump-era pandemic...
-


Politics
Trump says Prince Harry is “whipped” by Meghan Markle and the queen should have stripped them of their titles
Piers Morgan’s blockbuster interview with Donald Trump will air tonight in the UK, and the former...
-


Politics
Florida’s Disney district crackdown may violate the First Amendment: ‘highly likely to be unconstitutional’
One law professor said if the bill was a direct result of Disney’s political speech, it’s...
-


Politics
Man dies after setting himself on fire outside the Supreme Court Building
A climate activist who set himself on fire outside the United States Supreme Court Building on...
-


Celebrities
Donald Trump Issues Statement Following ‘Piers Morgan Uncensored’ Interview Storm Out
After walking out of Piers Morgan’s new talk show, Donald Trump has spoken out. It’s only...
-


Politics
Hillary Clinton filed a motion to dismiss Trump’s Lawsuit against her as having “no merit”
Hillary Clinton filed a motion on Wednesday seeking to dismiss former President Donald Trump’s lawsuit against...
-


Politics
Psaki Extends Doocy Feud As Biden Prepares To Appeal Mask Ruling, Doocy Dared To Challenge Inconsistencies of Biden Administration’s Mask Mandates
Psaki Extends Doocy Feud As Biden Prepares To Appeal Mask Ruling, Doocy Dared To Challenge Inconsistencies...
-


Politics
Department of Education Announce Changes: Millions of Individuals Closer to Student Debt Forgiveness under New Biden Administration
The Department of Education announced changes on Tuesday that are expected to bring millions of individuals...
-


Politics
Christian Music on Plane sparks outrage and Ilhan Omar is Criticized for Mocking a Video
People have criticized Minnesota Rep. Ilhan Omar for mocking a video of plane passengers singing. To...
-


Politics
Pelosi Drags Latinos Under the Bus in Battleground District
‘There’s all this talk about Latino voters, but where are we talking about Latino candidates and...
-


Politics
McCarthy thinks Biden should have helped Ukraine sooner, despite Trump’s decision to withhold aid from the country in 2019
House Minority Leader Kevin McCarthy said Russia “probably” would not have invaded Ukraine if the US...
-


Politics
Rep. Upton of the Republican Party criticizes the ‘MTG Element,’ claims they make it ‘hard’ to govern
Representative Fred Upton, a Republican from Michigan, slammed the “MTG element,” referring to Republican Representative Marjorie...
-


Politics
Democrats and Biden are in Election Trouble Because the Reliable Hispanic vote is in Jeopardy: “We’ve just got to do it.”
Despite a string of poor polls, current polls show that President Joe Biden is having a...
-


Politics
Former First Lady Melania Trump pushed Donald Trump to support Dr. Oz in the Pennsylvania Senate Race
According to a story, former First Lady Melania Trump reportedly pushed her husband, former President Donald...
-


Politics
President Biden Announces Crackdown on ‘ghost guns,’ Reveals new ATF Pick
Recently, President Joe Biden and his ATF lackey declared new gun control rules, concerning so-called “ghost...
-


Politics
Ukrainians’ ‘last stand’ to battle for Mariupol as the city expected to ‘fall within 24 hours’ to Russia
The beleaguer and the strategic port city of Mariupol are looking to fall to Russian hands...
-


Politics
Ex-President Donald Trump Just Made an Absolutely Head-Scratching Endorsement
Donald Trump held a gathering/ demonstration in North Carolina on Saturday night, but it unusual theatrics...
-


Politics
Psaki denied giving the reason why Biden Wrote College Counsel Letter for Chinese Businessman’s Son
During a White House meeting Wednesday, Press Secretary Jen Psaki denied giving reasons why President Biden...
-


Politics
Secret Service is Taking Charge $30,000-a-Month Malibu Mansion to Safeguard Hunter Biden
President Biden’s remaining son, Hunter Biden, is living in a rented four-bedroom “resort-style” home in Malibu,...
-


Politics
Ivanka Trump Not ‘Talkative’, But Helpful In Jan. 6 Probe
Ivanka Trump gave evidence before the Jan 6 on Tuesday. 6 committees that I inquired about...
-


Politics
Mike Lindell, CEO of MyPillow, claims that TV stations refused to let him appear in his commercials
Mike Lindell, the CEO of MyPillow, claims that he has been barred from appearing in many...
-


Politics
President Zelensky Made a Speech at the 2022 Grammy Awards
The 44-year-old Ukrainian president – whose country is agonizing an existing military seizure launched by Russian...
-


Politics
Hillary Clinton says ‘More’ can be done to hurt Putin, help Ukraine: ‘Double down’
Prior Secretary of State Hillary Clinton on Sunday called on the U.S. and its allies to...
-


Politics
In the Midst of Economic Crisis, Biden’s Budget Invests Nearly $40 Billion to Fight Global Climate Change
‘The Biden budget has one-sixth of a page on the opioid epidemic followed by six pages...
-


Politics
Gaetz Enters ‘Laptop From Hell’ Into Congressional Record After Nadler Rescinds Objection
Has the FBI assessed whether Hunter Biden’s laptop could be a point of vulnerability, allowing America’s...
-


Politics
Trump likely to have Committed Election-related Crimes: Judge Asserted “more likely than not”
A federal judge has asserted it is “more likely than not” that former President Donald Trump...
-


Politics
Video: War Between Russia and Ukraine Turns Kharkiv Metro into a Bomb Shelter
Since the start of the invasion, Russian forces have shelled Kharkiv’s residential structures and essential infrastructure....
-


Politics
Ukrainian Politician Says Country Will Not Remain Silent about ‘Horror of Rapes’ Against Women during Invasion
According to a Ukrainian legislator, Ukraine would “not be silent” about the “horror” of rapes committed...
-


Politics
Dr. Jill Biden has Devised new Rules in preparation for a White House
With these New Rules, Dr. Jill Biden gets even pettier: she felt “second class” Dr. The...
-


Politics
A New Poll adds to Good news for GOP and Trump in Years 22, 24
A new Emerson University polling shows lots of good news for Republicans in the run-up to...
-


Politics
President Joe Biden Will Visit Poland on Europe Trip This Week
As Russian forces concentrate their fire on cities and trapped residents in a nearly month-old invasion...
-


Politics
Khalid Payenda’s Journey from Afghan Finance Minister to Uber Driver in Washington
Khalid Payenda told The Washington Post he has been haunted by the fall of Afghanistan to...
-

Politics
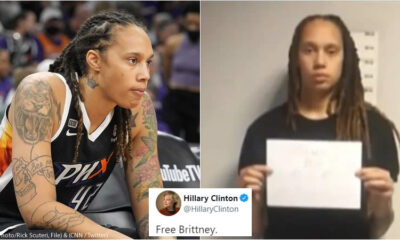
Hillary Clinton Joins Call on Twitter to ‘Free Brittney’ After Brittney Griner’s Arrest in Russia
Hillary Clinton has joined the call to bring home Phoenix Mercury star Brittney Griner. Following Griner’s...
-


Politics
President Joe Biden references Vladimir Putin as a ‘war criminal’
It is the first time the US President has used the remark in reference to Mr....
-


Politics
Donald Trump’s close friend and New York Jets owner, Woody Johnson wants to buy Chelsea
Woody Johnson is one of the numerous parties to emerge as potential owners of Chelsea, with...
-


Politics
British Residents Who Take In Ukrainian Refugees into Their Homes Will Receive Large Monthly Payment
The payment will be made as a “thank you” to those who have shown their support....
-


Politics
Trump Lawyer Knew That Plan To Postpone Biden Certification Was Illegal, Emails Show
Despite the fact that the scheme was in violation of the Electoral Count Act, John Eastman...
-


Politics
Psaki and DeSantis official clash over a Covid vaccine recommendation for healthy children: “Absolutely not. … We know the science”
Jen Psaki, the White House press secretary, criticized Florida surgeon general Joseph Ladapo’s advice that healthy...
-


Politics
Russian spy says Ukraine war will be a ‘total failure,’ with a ‘collapse similar to fall of Nazi Germany’
A whistleblower described the war as a “total failure” that could only be compared to Nazi...
-


Politics
Elon Musk Tells Ukrainian President Zelensky More SpaceX Internet Stations are On the Way
It appears that in this more and more troubled world, all roads lead to Elon Musk,...
-


Politics
First Lady Jill Biden introduces Kamala Harris as ‘the president,’ then says she was joking
Although it isn’t the first time Kamala Harris has been referred to the President, the American...
-


Politics
Donald Trump, who has a Long History of Criticising NATO now Claimed Credit for its Existence
Former President Donald Trump, who has a long history of criticizing the North Atlantic Treaty Organization...
-


Politics
“Problem Is Not That Putin Is Smart, But Our Leaders Are So Dumb”: Trump
Donald Trump made an appearance at the CPAC Republican Convention Even though he is currently killing...
-


Politics
Oil Prices Jump, Shares Falls as Ukraine Crisis Escalates
After Russian President Vladimir Putin recognized the independence of rebel-held regions of Ukraine, oil prices about...
-


Politics
First Lady Dr. Jill Biden is Redecorating Her East Wing Office with Mark Sikes: where she can hold larger meetings and host guests
The first lady’s office says the “project will be funded through donations to the White House...
-


Politics
Fox News Contributor admits to Fabricating a Story about Canadian woman being Trampled to Death
During ongoing trucker-led protests, Fox News contributor Sara Carter has pulled back her entirely fictitious story...
-


Politics
Joe Biden and Vladimir Putin Agreed to Meet over Ukraine Crisis on the Condition
Russia-Ukraine Crisis: The summit, proposed by France’s Emmanuel Macron, will be expanded to relevant stakeholders to...
-


Politics
Republican-controlled Florida House Passes a 15-week Abortion Ban
Republicans in Florida’s House of Representatives approved a 15-week abortion ban early Thursday, tightening access to...
-


Politics
The ‘Truth Social’ of Donald Trump Has Been Revealed—It Looks Almost Identical to Twitter
Donald Trump Jr. has shared online what is believed to be a screenshot of his father’s...
-


Politics
Hillary Clinton pushed Trump-Russia theory at the center of John Durham Case
Former President Donald Trump accused Hillary Clinton’s campaign operatives of spying on him and suggested they...
-


Politics
Trump Used Secret Service Agent’s Phone to Contact his Wife after Being Accused of Adultery
After being accused of adultery by the adult movie star, former US President Donald Trump used...
-


Celebrities
Katharine McPhee Criticizes Stacey Abrams for Photo without Mask with Schoolchildren: ‘The Hypocrisy Continues’
Despite a requirement, Katharine McPhee joined Stacey Abrams’ opponents in criticizing her for posing without a...
-


Politics
Palin v. New York Times Raises Concerns about Media Libel Laws
“The 360” shows you diverse perspectives on the day’s top stories and debates. The defamation case...
-


Politics
Fauci Declares ‘Full Blown’ Pandemic Phase Of Covid-19 Is Almost Over In US
Over the last three weeks, the number of persons in hospitals with COVID-19 has decreased by...
-


Politics
A new report adds to the mystery surrounding Melania Trump’s recent NFT auction
Vice reported on Tuesday about a strange series of transactions surrounding the auction for former First...
-


Politics
White House blasts Florida Republicans for their ‘Don’t Say Gay’ Bill
The White House has chastised the Florida Republican Party over legislation dubbed the “Don’t Say Gay”...
-


Politics
Trump illegally ripped up ‘hundreds’ of documents despite warnings, many of which were destroyed in ‘burn bags’
The Washington Post reported Saturday that former President Donald Trump tore up “hundreds” of White House...
-


Politics
Gaetz Friend Requests Judge For Sentencing Delay As He Works With Feds
A former Florida tax collector whose arrest led to a federal investigation into U.S. Rep. Matt...
-


Politics
Leaked documents raise new concerns about Biden administration’s preparations for withdrawal from Afghanistan: Report
On Tuesday, the Biden administration’s handling of the withdrawal from Afghanistan came under new scrutiny after...
-


Politics
Senator Lindsey Graham Mocked By Critics After Trump Turns On Him
Senator Lindsey Graham (R-SC) was mocked on Tuesday by his critics after his years of allegiance...
-


Politics
Paper Tantrum? Documents Subpoenaed by 6 Jan. Trump Reportedly Torn Panel
The documents were obtained by the 6 January Committee after a lengthy legal battle with the...
-


Politics
Democrat Workers Turn on Nancy Pelosi, Charles Schumer in Surprising New Survey
According to a surprising new survey, the vast majority of Democrat workers on Capitol Hill appear...
-


Politics
Pence’s Chief of Staff Marc Short Met With Jan 6th Committee
Marc Short, former Vice President Mike Pence’s chief of staff, has answered questions from the House...
-


Politics
What Does Kamala Harris’s Interview Responses Actually Mean? Body Language Expert Reveals
What Does Kamala Harris’s Interview Responses Actually Mean? Body Language Expert Reveals It is claimed that...
-


Politics
If prosecutors investigating him ‘do anything illegal,’ Trump threatens a “biggest protest we have ever had” in Washington, DC, and other cities
Former President Donald Trump called for nationwide protests at a rally in Texas if prosecutors investigating...
-


Politics
Donald Trump Stated that if he is re-elected President in 2024, he will Pardon Capitol Rioters
Former US president Donald Trump has promised to pardon the Capitol rioters if he makes it...
-


Politics
Sarah Palin Talks About Her Second COVID-19 Diagnosis
Sarah Palin said she felt “totally fine” in her first interview since contracting COVID-19 again on...
-


Politics
Trump Mocked for an Embarrassing ‘Please Clap’ Moment at his own Resort
The former president seemed to need some adulation at Mar-a-Lago. Donald Trump might have had his...
-


Politics
Trump Dismisses Rumors Of Feud with DeSantis: ‘We Have A Good Relationship’
Former President Donald Trump dismissed reports of a growing feud between himself and Florida Gov. Ron...
-


Politics
All of Biden’s successes or failures, it’s really about ‘COVID, stupid’
President Biden held a nearly two-hour, wide-ranging news conference on Wednesday that, for all of its...
-


Politics
Riley Roberts is Alexandria Ocasio-longtime Cortez’s Partner whom She Met in College
Alexandria Ocasio-Cortez, a New York Representative, is known for making headlines, whether for her strong opinions...
-


Politics
Gaetz’s ex-girlfriend is Granted Immunity in S*x Trafficking Investigation
The sex trafficking case against Rep. Matt Gaetz (R-FL) is surging after it was revealed on...
-


Politics
Trump Claims that White People are Discriminated against when it comes to COVID-19 Treatment: ‘If you’re white, you go to the back of the line’
Former President Donald Trump claimed on Saturday during a rally in Florence, Arizona, that white people...
-


Politics
Melania Trump’s Item Auction Is ‘Basement-Level Tacky…She Needs Money,’ Says ‘The View’ Hosts
The ladies of The View have slammed Melania Trump‘s recent antics. The former First Lady has...
-


Politics
Candace Owens promotes a vaccine conspiracy theory in connection with Bob Saget’s death
Candace Owens, a far-right troll, suggested on Tuesday that beloved comedian Bob Saget may have died...
-


Politics
Donald Trump Cut NPR Interview After His “Rigged” Election Idea Debated
When the main focus is on Donald Trump, he can’t even handle it. Trump appeared on...
-


Politics
Congresswoman Requests Capitol Police Help While Expressing ‘Concerns’ About Rep. Greene’s ‘Mental Health’
Rep. Haley Stevens (D-MI) has asked for help from Capitol Police after Rep. Marjorie Taylor Greene...
-


Politics
Hunter Biden’s ‘Close Friend’ Arrested in Kazakhstan For Treason
In one meeting, which took place in Kazakhstan, Hunter Biden ditched his Secret Service security detail...
-


Politics
What Is Voting Rights Filibuster? New Agenda of Joe Biden
US Senate: The popular perception of a filibuster involves a lone senator speaking for hours and...
-


Politics
Biden will take a “forceful” Push for Voting rights and Filibuster Reform in his Speech in Georgia
With less than 10 months until the 2022 midterm elections, President Joe Biden will travel to...
-


Politics
Romney Defends Biden’s 2020 win after Trump Criticizes the GOP’s Rounds
Following an attack by former President Donald Trump, Republican Senator Mitt Romney of South Dakota defended...
-


Politics
Michelle Obama’s guest appearance on ‘Black-ish’ excites fans
Michelle Obama made a guest appearance on Tuesday’s eighth and final season premiere of Black-ish, after...
-


Politics
With the help of your tax return, get $1,400 in stimulus checks
Taxpayers can receive up to $1,400 in stimulus checks through their tax returns at the start...
-


Politics
Lauren Boebert Comes to Marjorie Taylor Greene’s Help After Twitter Ban, And Things Don’t Go Well
Rep. Lauren Boebert (R-Colo.) caused outrage with her threatening reaction to Twitter’s suspension of fellow far-right...
-


Politics
Stephen Colbert Reveals Unseen Trump Footage From January 6th That He Hopes Will Be Released Next
Stephen Colbert expected that the world would soon see what Donald Trump was up to during...
-


Politics
CNN Opinion Columnist: ‘Let’s Go Brandon’ Dad Deserves To Have Life Ruined
‘Apparently, he thinks he should be able to tell Biden to basically go fk himself while...
-


Politics
Joe Biden criticizes Evils of Big Meat in Bizarre, Senile Performance
This morning, RedState reported on Joe Biden’s plan to avoid blame for the nation’s inflation crisis,...
-


Politics
Members of House Select Committee Verifies Communications between Ivanka and Donald Trump during Capitol Siege, Says They Have “Critical Testimony” About Interactions
Members of the House Select Committee looking into the deadly Capitol insurgency on January 6th stated...
-


Politics
Jen Psaki’s Favourite Phrase Could Be Banned Soon
According to Lake Superior State University‘s renowned annual list of banned terms, there should be no...
-


Politics
Trump Slams Comcast and NBC Executives as “Terrible Human Beings…just disgusting”
Former President Donald Trump appeared on the conservative YouTube channel Right Side Broadcasting and expressed his...
-


Politics
Melania Trump Records Kids’ Birthday Messages and Wrote Inspirational Letter to High School Students
• She has grandparent responsibilities to her stepchildren Ivanka, Eric, and Donald Jr., but she’s also...
-


Politics
Bill Clinton Story 2021: Getting $120 Million Divorce After Health Crisis
Is Invoice Clinton planning to divorce Hillary? Though the tabloids spread multiple rumors about the Clintons...
-


Politics
‘Who gives a f***,’ Melania Trump Said in a Foul-mouthed Christmas Rant
During her four years in the White House, Melania Trump received a lot of backlash for...
-


Politics
Trump’s spokesman says that he has cooperated with House panel investigating events of January 6th
In a court filing on Friday, a current spokesman for former US President Donald Trump said...
-


Politics
Staffers working under Biden are considering leaving the White House due to “poor management”
According to confidential and anonymous conversations with Biden White House staffers, Politico’s West Wing Playbook says...
-


Politics
Pelosi frustrated by chants of “Let’s Go Brandon” in her own far-left district
Fox News reported swamp monster and career politician, Nancy Pelosi, D-Calif., was overwhelmed by her own...
-


Politics
Biden claims that Americans are better off than they were years ago
The desperate Brandon administration attempted to convince Americans that, despite overwhelming evidence to the contrary, they...
-


Politics
Joe Biden gets double hit from Manchin and another Covid winter
Democratic Sen. Joe Manchin dropped the ax on his party’s agenda on Sunday, saying he would...
-


Politics
Fourth Stimulus Check: Criteria for Receiving $1,400 Payment in 2022
Some people in the United States of America can look forward to receiving a payout of...
-


Politics
South Dakota Governor Kristi Noem holds push to Prohibit Transgender Women and Girls from Engaging in Female Sports
South Dakota Governor Kristi Noem announced on Tuesday that she has proposed legislation in her state...
-


Politics
‘Why Is Anybody Surprised?’ Democratic Congressman Rips ‘Traitor’ Jim Jordan Over Jan. 5
Rep. Jim Jordan has marked a “traitor to the Constitution” by Rep. Ruben Gallego (D-Ariz) after...
-


Politics
Liz Cheney raised the possibility of Trump election crime
Andrew McCabe, the former deputy director of the FBI, and David Williams, the former inspector general...
-


Politics
Federal Court Will Consider Overturning Injunction against Joe Biden’s Vaccination Mandate
‘While I would have much preferred that requirements not become necessary…’ (The Center Square) – A...
-


Politics
Trump Rally Features ‘Many Empty Seats’ — Prompting Organizers to Close Arena’s Top Level
On Saturday, organizers had to close the top bowl of the arena because there were so...
-


Politics
Piers Morgan tells Hillary Clinton to let it go! Trump Loss Meltdown after 2016
Earlier, an emotional ex-presidential candidate Hillary Clinton almost turned on the waterworks while reading her would-be...
-


Politics
Sunrise’s Co-Host Natalie Barr Shares her Embarrassing Story about Phone Call With the ‘Well-Hung Guy’
On Wednesday, Natalie Barr, co-host of Sunrise, told the team a hilarious story about a recent...
-


Politics
Stacey Abrams is still Lying about the Georgia Election, she Refused to Accept Defeat
‘Concession means to acknowledge an action is right, true, or proper…’ Stacey Abrams, a failed gubernatorial...
-


Politics
Will Epstein’s Rich & Powerful Friends Be Revealed in the Maxwell Trial, or Will It Be Another Cover-Up?
On November 29, the trial of convicted sex offender Jeffrey Epstein’s close confidant Ghislaine Maxwell starts....
-


Politics
Biden Launching Urgent Campaign for Americans to Get COVID-19 Booster Shots
Private insurers will be required to cover the cost of at-home Covid-19 tests, and testing procedures...
-


Politics
As Joe Biden Snubs Hungary, Viktor Orbán Fears Election Interference
The Hungarian government voiced concern that the US would try to intervene in their elections after...
-


Politics
House Panel Subpoenas Trump supporters Roger Stone and Alex Jones in Capitol Riot Inquiry
A committee looking into the US Capitol insurgency has subpoenaed five more people, including former President...
-


Politics
AOC Claims It Was A ‘Mistake’ For Dems Not to Ask For Her Help in Va. Elections
Not a single person asked me to send an email, not even to my own list…’...
-


Politics
Biden Mocked For ‘Ron Burgundy’ Moment after Sticking to Script in Speech
According to right-wing critics, US President Joe Biden had a ‘Ron Burgundy’ mix-up with a teleprompter. ...
-

Politics
Bill Maher Rejects Critical Race Theory, Claiming That Racism Isn’t In America’s DNA
Bill Maher, a comedian, and television host expressed sympathy for parents’ concerns over critical race theory...
-


Politics
Biden Administration Offering more Aid for Winter Heat, Utility Bills
The Biden administration is taking steps to help distribute several billion dollars in winter heating and...
-


Politics
President Biden says reversing High Inflation “Top priority” As US Prices hit 30-years High
President Joe Biden has said that fighting inflation in the United States is his “top priority”...
-


Politics
Log Cabin Republicans Move their Annual Gala to Florida to Honour Melania Trump
Donald Trump is expected to attend the Log Cabin Republicans’ annual Spirit of Lincoln dinner, which...
-


Politics
Kellyanne Conway Returns with Her Most Brazen Trump Lie Yet
Former Counselor to the President of the US Kellyanne Conway resurfaces on Fox News to attack...
-


Politics
President Biden Repeatedly Claims he’ll be in ‘trouble’ for Taking Press Questions
Following remarks about the passage of the $1.2 trillion infrastructure bill, President Biden warned he would...
-


Politics
Chinese Tennis Star Peng Shuai Claims China’s Former Vice Premier Forced Her into S*x
Peng Shuai, the former world No. 1 tennis doubles player, claimed in a Weibo post that...
-


Politics
House Democrats restored paid family leave in the social safety net bill after Biden removed it to please the right-wing
Nancy Pelosi, US House Speaker, announced changes in a Wednesday letter to her colleagues, saying it...
-


Politics
Glenn Youngkin Republican beats McAuliffe for the governorship of Virginia
Republican Glenn Youngkin defeated Democrat Terry McAuliffe in Virginia’s gubernatorial election Tuesday night, striking a political...
-


Politics
Biden Apologizes to World Leaders for Trump’s Exit from Paris Accords at COP26
President Joe Biden was criticized on Monday after he seemed to close his eyes and nap...
-


Politics
Is This Biden Policy is About to Create another National Crisis
Biden is good at one thing: performing a terrible job, and he’s about to create another...
-


Politics
Ex-New York Governor Andrew Cuomo Charged With Misdemeanor S*x Crime
Former New York Governor Andrew Cuomo has been charged with a sex crime in Albany City...
-


Politics
Florida Sues Biden, NASA over “Unlawful” COVID-19 Vaccine Mandates for Federal Contractors
A lawsuit claims that a federal rule interferes with Florida’s employment policies. President Biden, NASA, and...
-


Politics
Jen Psaki Bombs Christian Reporter Who Compared Abortion to ‘Hiring a Hitman’ ‘I Answered Your Question’: WATCH
It’s always interesting to see reporters try to one-up White House Press Secretary Jen Psaki as...
-


Politics
Is Kamala Harris Keeping a safe Distance from Biden as his Popularity Plummets?
The poll results continue to give a clear picture of the American people’s feelings toward Joe...
-


Politics
Merrick Garland denies Republicans access to January 6 records – Tells them to go beg Nancy Pelosi
The Department of Justice, led by openly partisan Attorney General Merrick Garland, has advised House Republicans...
-


Politics
Prince Andrew’s Lawyer Wants to Keep 2009 Legal Deal Sealed
Virginia Giuffre, the royal’s accuser, sued millionaire Jeffrey Epstein and his life partner Ghislaine Maxwell in...
-


Politics
State Department will Establish a new Cyberspace Bureau to Tackle Online Attacks
Changes are part of the Biden administration’s approach to cybersecurity as a critical national security issue....
-


Fitness
Fauci Under Fire For Alleged Puppy Experiments That Saw Beagles Kept In Cage To Be Eaten By Hungry Sandflies
DR. Anthony Fauci has come under criticism for allegedly supporting research in which beagle puppies were...
-


Politics
What’s Behind the Push for a Fourth Stimulus Payment
The IRS distributed more than 169 million payments in the third round of direct stimulus aid,...
-


Politics
Congressional Investigators Found The Trump Administration Used Its Food Aid Program for Political Gain
A $6 billion federal program created to give fresh food to families affected by the pandemic...
-


Politics
CNN’s journalist, John King announces he’s been battling MS for years live on air
John King, a CNN journalist known for his in-depth election night coverage, revealed for the first...
-


Politics
Liz Cheney Approaches GOP Colleagues Ahead of Bannon Contempt Vote: ‘You All KNOW’ Election Fraud Claims Are False
Liz Cheney, the U.S. Representative for Wyoming, sent a strong signal to her Republican colleagues on...
-


Politics
Trump to be Deposed in a Lawsuit Filed by Protestors Claiming Assault by his Security Guards
Former President Donald Trump is ordered to submit testimony next week under oath Monday in a...
-


Politics
Jill Biden ex-husband Questioned ahead Durst Grand Jury
Just since Wednesday afternoon, the long-running Robert Durst murder has taken an intriguing turn. According to...
-


Politics
Donald Trump is bookmakers favorite to win the 2024 US Presidential election
For the first time since before the November 2020 presidential election, two leading bookmakers have placed...
-


Politics
Stephanie Grisham says she naively thought she and Melania Trump were ‘Friends’
Stephanie Grisham was surprised when Melania Trump stopped speaking to her, following her resignation, she told...
-


Politics
Senate Report Documents, Trumps Effort to Manipulate the Justice Department
Former President Donald Trump has informed 4 former senior advisors not to worry about a federal...
-


Politics
Trump falsely claims Haitian immigrants entering the US ‘probably have AIDS’ and allowing them in is like a “death wish”
Trump falsely claims Haitian immigrants entering the US ‘probably have AIDS’ and allowing them in is...
-


Politics
Trump criticizes McConnell, says he gave Democrats a “lifeline”
Former U.S. President Donald Trump criticized Addison Mitchell McConnell, Senate Minority Leader, for giving Democrats ‘a...
-


Politics
Judge Orders Texas to Suspend Enforcement of Abortion Law
A federal judge has temporarily halted Texas’ restrictive Senate Bill 8. After the Justice Department argued...
-


Politics
Trump falls off Forbes list of 400 richest Americans for the First Time in 25 Years
Forbes has released an annual ranking of the wealthiest 400 Americans since the early 1980s. Former...
-


Politics
Former White House Press Secretary Stephanie Grisham Warns ‘Trump will seek revenge’ if re-elected
Former White House press secretary Stephanie Grisham has warned that if Donald Trump runs again and...
-


Politics
Melania Trump Had Google Alerts SetUp So She could Be “reading every little thing written” about her: Book Claims
According to Grisham’s forthcoming book, “I’ll Take Your Questions Now,” First Lady Melania Trump was reportedly...
-


Politics
Biden Signs Bill to Avoid Partial Government Shutdown
President Joe Biden signed legislation to avoid a partial federal shutdown and keep the government funded...
-


Politics
Phil Murphy’s New TV Ad Links Ciattarelli and Trump Comments on Children Getting Covid-19
Gov. Phil Murphy’s re-election campaign has released a new TV ad linking Republican opponent Jack Ciattarelli’s...
-


Politics
Trump turned down a charity challenge to go vegan for a month because he bizarrely said it would kill his brain cells
According to a new book, former President Donald Trump turned down a dare from a nine-year-old...
-


Politics
Former U.S. Soldier Arrested For Breaching Capitol Grounds On Jan. 6 In Full Tactical Gear
Jeremy Brown, a former United States Army Special Forces soldier who ran for Congress as a...
-


Politics
Melania Trump Allegedly Found Small Ways to Strike Back at Donald Trump For His Affairs Coming to Light
Melania Trump has been through a lot during her marriage to Donald Trump. While she’s no...
-


Politics
Ashley Moody Urges Congress to Pass Vern Buchanan’s Cop Killer Punishment Bill
Florida Attorney General Ashley Moody and U.S. Rep. Vern Buchanan, R-Fla., joined forces this week to...
-


Politics
Ivanka Trump and Jared Kushner tried to attend Meeting with Queen Elizabeth II during a State Visit, new book claims
Ivanka Trump and Jared Kushner tried to attend a meeting with Queen Elizabeth II but were...
-


Politics
Biden-Harris Administration moving to Protect Dreamers after Texas court ruling
After a federal court in Texas recently dealt a major blow to the Obama-era rule, the...
-


Politics
Texas Governor Greg Abbott Defends upcoming 2020 Election Audits that Trump Demanded
On Sunday, Texas Governor Greg Abbott defended his state’s upcoming audit of presidential election 2020 results...
-


Politics
White House Advises Federal Agencies to Prepare for first Government Shutdown of Pandemic
The U.S. government has advised federal agencies to prepare for a possible shutdown, as the White...
-


Politics
Trump Sues Niece, NY Times Over Records Behind 2018 Tax Story
Time to reset the clock: After dozens of empty threats, Donald Trump has followed through on...
-


Politics
Obama told Trump that he couldn’t recall his biggest mistake, According to The book “Peril”
According to a new book, Trump asked Obama to disclose his biggest mistake. This happened when...
-


Celebrities
Arnold Schwarzenegger Says The State ‘Made The Right Decision’ Not To Recall Newsom
Former California Governor Arnold Schwarzenegger said that California “made the right decision” in not recalling Governor...
-


Politics
Trump-Appointed Special Counsel Accuses the Lawyer with Links to Hillary Clinton
As the investigation into the origins of the FBI’s Russia probe continues, a private lawyer with...
-


Politics
United Nations Special Envoy Meets New Afghan Interior Minister Wanted By US
A United Nations representative met with Afghanistan’s new interior minister, who was one of the world’s...
-


Politics
Antony Blinken Defends Afghan Withdrawal at U.S. Congressional Hearing
US Secretary Of State Antony Blinken Defends Afghan Withdrawal And Blames Trump Administration Taliban Agreement At...
-


Politics
US Marks Milestone Anniversary of 9/11
The 9/11 anniversary commemoration at ground zero has begun with a tolling bell and a moment...
-


Politics
Donald Trump Contacted Families Of US Troops Killed In The Kabul Terror Attack
Donald Trump contacted the families of US troops that were killed in the Kabul Airport suicide...
-


Politics
Justice Department Takes Steps For Protecting Texas Women Seeking to Terminate Unwanted Pregnancies
US Attorney General Merrick Garland declared that the Justice Department is ready to assist Texas women...
-


Politics
Prince Charles’ Royal Aide Michael Fawcett Steps Down As Head Of Charity Amid ‘Golden Visa’ Allegations
Mahfouz Marei Mubarak bin Mahfouz, a Saudi Arabian billionaire, is said to have paid tens of...
-


Politics
VP Kamala Harris to Campaign With Gavin Newsom In Final Stretch Before California Recall Election
Vice President Kamala Harris will campaign with California Governor Gavin Newsom in the Bay Area on...
-


Politics
Trump-appointed ambassador Kelly Craft Directed Government Business to his Hotel
US businesswoman and political donor Kelly Craft steered government business to then-President Donald Trump’s Washington, D.C.,...
-


Politics
Monica Lewinsky Pleased with The Many Apologies to Britney Spears and Says It’s ‘Long Overdue’
Monica Lewinsky, whose infamous affair with President Bill Clinton while working as an unpaid intern at...
-


Politics
Supreme Court Declines to Block Texas Abortion Law
The Supreme Court late Wednesday declined to halt a law banning abortions as early as six...
-


Politics
White House defends letting billions in military equipment fall into Taliban hands
White House press secretary Jen Psaki claimed Monday that the Biden administration had no intention of...
-


Politics
EU recommends new Travel Restrictions for U.S. Tourists as Covid Cases Rise
Covid-19’s Delta variant is proliferating worldwide threatening unvaccinated populations and economic recovery. The Council of the...
-


Politics
President Joe Biden pays respects to US troops killed in Afghanistan
The remains of 13 US soldiers killed in an attack at Kabul airport last week are...
-


Politics
Judge Orders Sanctions Against Sidney Powell, Other Lawyers Who Filed Lawsuit Challenging 2020 Election
In Michigan, a federal judge has ordered sanctions against former Trump attorney Sidney Powell, attorney Lin...
-


Politics
Donald Trump-backed Herschel Walker seeks Georgia Senate seat
After months of speculation, Herschel Walker filed paperwork to run for the United States Senate in...
-


Politics
Kathy Hochul Becomes The First Female Governor Of New York
Kathy Hochul, a former lieutenant governor, was sworn in as New York’s first female governor at...
-


Politics
North Carolina Lawmakers Considers Raising Minimum Marriage Age From 14 to 16
North Carolina is one step closer to raising the minimum age from 14 to 16 to...
-


Politics
Biden Announces Student Loans Cancellation of $5.8 Billion for Disabled Under TPD Discharge Program
On Thursday, the Biden administration announced that 323,000 debtors will have their federal student loan debt...
-


Politics
Chris Cuomo Finally Breaks Silence Over Andrew’s Scandal and Says He Urged His Brother to Resign
Chris Cuomo finally broke his on-air silence over his brother’s s*xual harassment issue and subsequent resignation...
-


Politics
Rand Paul’s YouTube Account Suspends After Providing Misinformation About COVID-19 Mask
After posting a video saying most masks are ineffective in combating COVID-19, YouTube has suspended Republican...
-


Politics
‘JEOPARDY!’ Champion Austin Rogers Expresses His Opinion About New Host Mike Richards
One of the most famous “Jeopardy!” champions of all time has strong thoughts about the new...
-


Politics
Alexandria Ocasio-Cortez Occasionally Watch Fox News Coverage of Her: She Says ‘It’s Really Fascinating’
Representative Alexandria Ocasio-Cortez (D-NY) spoke with CNN’s Dana Bash for the first episode of the new...
-


Politics
Trump Issued Statement Endorsing Jesse’s Book, Plagiarizes His Review from Book’s Details Page
Former President Donald Trump issued a statement today endorsing Jesse Watters’ book, “How I Saved the...
-


Politics
Andrew Cuomo Refuses to Resign And Denied Allegations Against Him
Andrew Cuomo, a sexual predator and the governor of New York, spoke out at an emergency...
-


Politics
Joe Biden Finally Denounce New York Governor Andrew Cuomo
The pressure on Joe Biden to finally criticize New York Governor Andrew Cuomo grew too much...
-


Politics
Donald Trump’s Unusual Relationship with His Children
Donald Trump’s connection with his children is strange, to say the least, and each of them...
-


Politics
Barack Obama Throwing Birthday Party While Defying CDC Guidelines
Barack Obama is celebrating his 60th birthday this week. His long guest list is being attacked for...
-


Politics
“You’re Not as Smart as I Thought You Were,” Biden remarks of unvaccinated Americans
Biden stated, during a press conference on Tuesday, while walking away from the podium that the...
-


Politics
Kristi Noem Again At Fault, This Time Attacked Ron DeSantis at CPAC
Kristi Noem beautiful, articulate, and talked a tough game is surely a rising star in the...
-


Politics
OANN Witnessed One More “Glitch” in The Joe and Kamala “Simulation”
Another “bug” in the Biden mockup? Several people sense as if Team Biden isn’t trying to...
-


Politics
Watch: Jim Acosta Thought He Could “Man Handle” Rep Cawthorn…Boy, Was He Wrong…
Jim Acosta supposed he had a “slam-dunk” working after Rep Cawthorn…But instead, Acosta got SOAKED ON...
-


Politics
Melania Spotted While Exiting From Trump Tower While Carrying A 20K Purse As Indictments Knockout Donald’s Organization
Humiliated ex-president Donald Trump is going over it in the wickedest kind of way these days...
-


Politics
Trump Appeared In A News Show and Thought He’s Still President Claimed People
Donald Trump has lost all reputable social media platforms to express himself because nobody will read...
-


Politics
Barack Obama Revealed Malia Believed 4th July Fireworks Were For Her
Barack Obama and Michelle Obama recalled their daughter, Malia, on her birthday by honoring her on...
-


Politics
Donald Trump Is Ahead to Take His Revenge on Obama
Derrick Watson, the Obama-appointed judge from Hawaii who jolted off the entire “activist judge” conspiracy screw...
-


Politics
More Losses For Biden Ahead, Now Keystone Pipeline is Taking Place
More Losses For Biden Ahead, Now Keystone Pipeline is Taking Place. Team Biden can’t get a...
-


Politics
Keir Starmer Used Clinton’s Slogan To Show The Togetherness
In May, Keir Starmer, the UK Labour Party leader, swore that the UK Labour Party s...
-


Politics
Joe Biden Openly Retreat Hypocritical Republicans List
Only a few Republicans advertised the $1.9 trillion American Rescue Plan after they voted against it....
-


Politics
Ivanka, Jared Created Fake Credentials To Save Trump: Proofs
Michael Cohen who is Donald Trump’s old personal attorney and self-described “fixer” is again in limelight,...
-


Politics
The Americans Are Not Ready To ‘Move On’ Over The Election Unfairness
Cheaters may prosper for a short time, but they won’t win in the long run says...
-


Politics
Pence does not see ‘eye to eye’ with Trump on US Capitol Riot
A ‘dark day’ in US history, but the former vice president is still ‘proud’ of his...

